Iceland is a registry-rich country with a small enough population that genuinely nationwide health data is feasible — not the survey-based approximations that anchor most psychiatric epidemiology elsewhere. A 2026 PLOS One study used the Iceland Screens, Treats, or Prevents Multiple Myeloma (iStopMM) cohort — 80,759 adults aged 40+, representing 54% of all eligible Icelanders — to map psychiatric diagnoses, medication use, and symptom burden against population data.
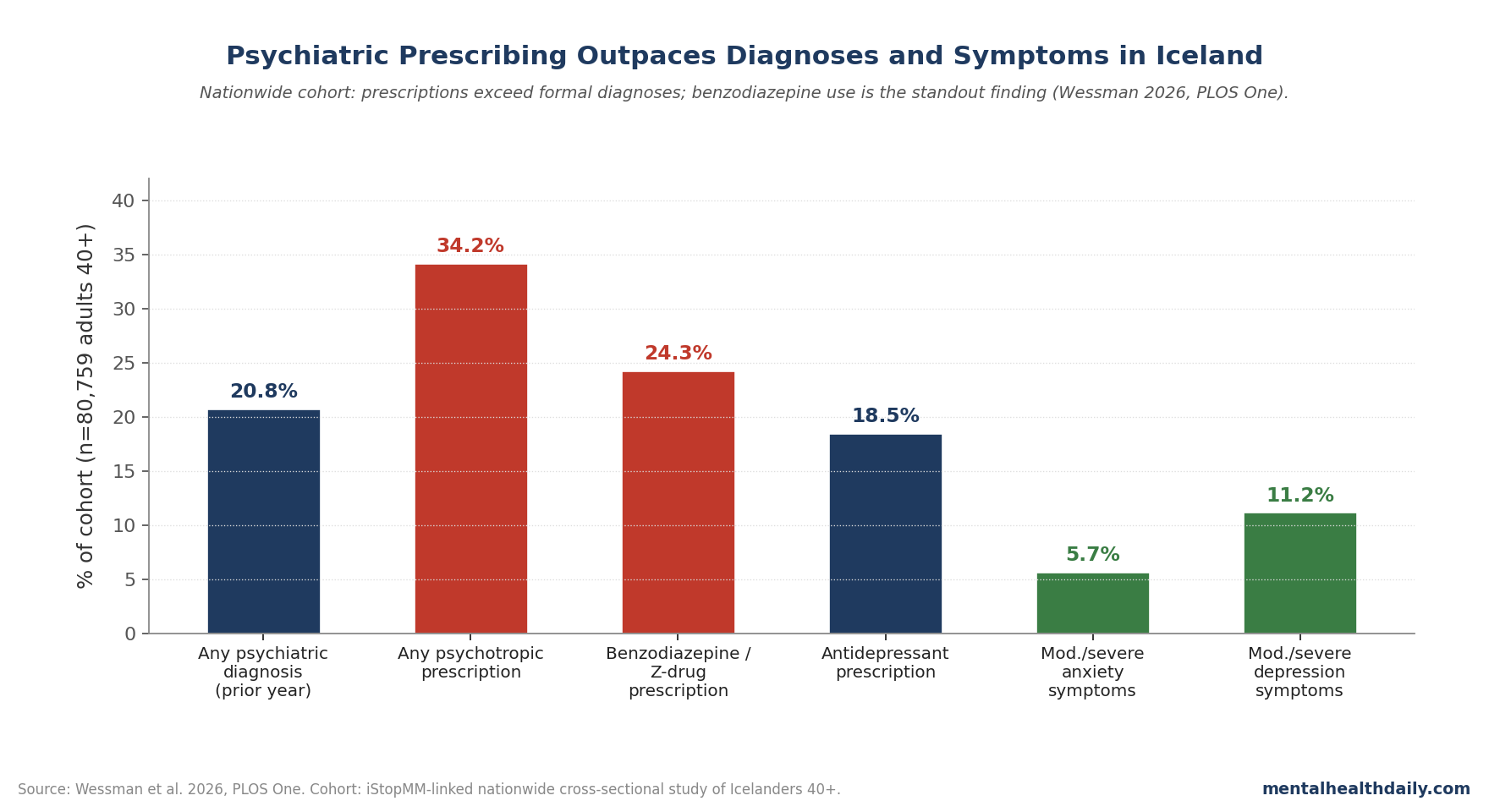
The main numbers are unsettling. 20.8% had at least one psychiatric diagnosis in the year before enrollment. 34.2% filled at least one psychotropic prescription — meaning roughly a third of mid-life and older Icelanders were on psychiatric medication. 24.3% filled benzodiazepine or benzodiazepine-related prescriptions. And 19.9% of those filling psychotropics did so without any formal psychiatric diagnosis.1
Research Highlights
- Cohort: 80,759 Icelanders aged 40+ (54.3% of eligible population), cross-sectional with linked national registry data.
- Diagnoses: 20.8% with ≥1 psychiatric diagnosis in the prior year; sleep disorders, anxiety disorders, and depressive episodes most common.
- Prescriptions: 34.2% filled ≥1 psychotropic; 24.3% filled benzodiazepine-related medications.
- Without diagnosis: 19.9% of those on psychotropics had no formal psychiatric diagnosis on record.
- Symptom burden: 94.3% no/mild anxiety; 88.8% minimal/mild depression; 59.3% satisfied with life.
- Age trend: Diagnosis and prescription rates rose with age across the 40+ range.
The mismatch between prescribing rates and self-reported symptom burden is the substantive finding here, and it’s worth taking seriously.
Iceland’s Registry Data Gets Closer to Real Psychiatric Prevalence
Population-level psychiatric statistics usually come from one of two sources, each with predictable problems. Survey data — the workhorse of cross-national comparisons — underrepresents people with active psychiatric illness, people in institutional settings, men, and younger adults. Registry data captures whoever interacts with the healthcare system but misses people who never present.1
The Wessman analysis combines both. The 80,759 participants are linked to national prescription, diagnosis, and hospitalization registries, and self-report symptom and life-satisfaction measures fill in the picture for people with subclinical or unrecognized illness.
For the 40+ population in a country with universal healthcare and a near-complete national registry, this is about as close to ground truth as psychiatric epidemiology gets.
Iceland-specific caveats apply. The country is small, ethnically homogeneous, and high-income with universal coverage; its prescribing patterns and treatment access don’t generalize to most of the world. But that’s precisely what makes the patterns interesting: in a system with low barriers to mental health care and high registry completeness, what does the steady-state look like?
Benzodiazepine and Z-Drug Use Reached 24.3%
One in four adults aged 40+ filled a benzodiazepine or benzodiazepine-related (Z-drug) prescription in the study window. That’s the finding the authors flag as “alarming,” and they’re right to.1
Benzodiazepines and Z-drugs are not first-line treatment for any common psychiatric disorder. Major guidelines — American Psychiatric Association, NICE, Australian RANZCP — list them as short-term adjuncts at most. The reasons are well-documented: tolerance and dependence, falls and fractures in older adults, cognitive impairment, increased dementia risk on long-term use, withdrawal complications, and modest benefit for chronic anxiety and insomnia compared to first-line alternatives.2
And yet the Iceland data shows a quarter of mid-life and older adults filling these prescriptions in a single year. The pattern is not unique to Iceland — it tracks high-income-country benzodiazepine prescribing trends going back decades — but the registry granularity makes the scale unmistakable.
Psychotropic Use Without Diagnosis Reached 19.9%
Roughly a fifth of psychotropic prescriptions in the cohort were filled by people without any formal psychiatric diagnosis on the registry. There are several plausible explanations, none of them clean:
- Diagnostic shorthand in primary care. A GP may treat anxiety or insomnia symptomatically without entering a formal diagnosis code. The patient gets the prescription but the registry shows no diagnosis.
- Medication for non-psychiatric indications. Some psychotropics are used off-label — tricyclics for chronic pain, SSRIs for premature ejaculation or hot flashes, antipsychotics for sleep or migraine. The registry shows the prescription; the indication isn’t psychiatric.
- Ongoing prescriptions from prior diagnoses. The diagnosis was recorded years earlier and isn’t flagged in the prior-year window the study used.
- Genuine over-prescription. Patients receiving psychotropics for vague symptom complaints without proper diagnostic workup.
The registry can’t distinguish these. What it can show is that a substantial fraction of psychotropic use happens outside the formal diagnostic framework that guidelines assume.
Symptom Burden Was Lower Than Prescribing Rates Would Predict
Cross-tabulating symptoms against prescriptions shows the most striking finding: most people on psychotropics didn’t have current moderate or severe symptoms. 94.3% of the cohort reported no or mild anxiety; 88.8% reported minimal or mild depression; 59.3% reported life satisfaction or extreme satisfaction.1
This isn’t necessarily a contradiction — treatment is supposed to reduce symptoms, and people on effective psychotropic therapy should report lower symptom burden by design. But the gap between 34% prescribed and roughly 6–11% with moderate or severe symptoms invites scrutiny.
Three explanations are on the table: psychotropics are working extraordinarily well at scale (possible but optimistic), a meaningful fraction of people are taking medication they don’t need (consistent with the prescription-without-diagnosis pattern), or the symptom measures capture only a snapshot that misses chronic distress.
Older Adults Carried the Highest Medication Risk
Diagnosis and prescription rates climbed steadily across age groups in the 40+ cohort. By the oldest brackets, prescription rates were higher still. This pattern matters clinically because benzodiazepine and Z-drug use in older adults carries amplified harms: cumulative cognitive effects, fall and fracture risk, and possible association with later dementia incidence.4
The Beers Criteria and STOPP/START guidelines have flagged benzodiazepines and Z-drugs as potentially inappropriate medications in adults 65+ for over a decade. The Iceland data shows that despite these guidelines, prescribing in older adults remains substantial in a high-income healthcare system.
Limits of the iStopMM Cohort: Volunteer Bias, Symptom Snapshots, ICD-10 Drift
Four caveats matter before treating these numbers as universal:
- Volunteer-based cohort. 54.3% of eligible Icelanders registered. The 45.7% who didn’t may differ systematically — people with active untreated illness, social isolation, or distrust of medical research are plausibly underrepresented, which would push the true prevalence higher than reported.
- Symptom measures are single-timepoint. Self-report anxiety and depression scales capture how a person feels in the assessment window, not over months or years. Chronic-but-currently-quiescent illness gets undercounted, and the symptom-vs-prescription gap may partly reflect treated patients in a stable interval rather than overprescription per se.
- ICD-10 codes carry clinical variability. The diagnosis registry reflects whatever GPs and psychiatrists entered in real practice, with all the documentation drift that implies. “Sleep disorder” from one clinician may overlap heavily with “adjustment disorder” from another.
- Iceland-specific norms don’t generalize. Cultural attitudes toward psychotropic use, prescribing conventions, and access barriers vary widely across countries. Iceland’s benzodiazepine rate is high relative to some European peers and lower than others — the directional pattern likely travels, but the absolute numbers don’t.
Deprescribing and Off-Diagnosis Prescribing Are the Action Points
Two findings travel beyond Iceland and shape the policy conversation:
- Benzodiazepine prescribing remains substantial despite decades of guidelines telling clinicians to avoid them as first-line and long-term agents. The gap between guideline and practice is wide enough that “deprescribing” is now a recognized clinical sub-discipline, with structured protocols for tapering long-term benzodiazepine users off the drugs.
- Registry-based prescribing outpaces diagnosis-based prescribing, suggesting pharmacotherapy for psychological distress is happening in a substantial gray zone outside the formal diagnostic framework guidelines assume. That doesn’t mean the prescribing is wrong — primary-care symptom management has its place — but policy discussions about psychotropic use need to engage with the off-diagnosis pattern, not pretend it doesn’t exist.
Questions About Population Psychiatric Epidemiology
Are the Iceland numbers higher or lower than other countries?
Roughly comparable to other high-income European countries. Sweden, Norway, and the UK report psychotropic prescription rates in similar ranges. Benzodiazepine rates vary more widely. The 21% diagnosed prevalence is consistent with WHO estimates for high-income countries.
Why does benzodiazepine prescribing remain high if guidelines discourage it?
Several reasons: rapid symptomatic relief that patients value, prescriber inertia for long-term users, limited access to first-line alternatives like CBT-I or therapy, and patient resistance to stopping medication that “works” in the short term.
Are Z-drugs (zolpidem, zopiclone) safer than benzodiazepines?
Marginally, but not as much as initially marketed. Tolerance, dependence, and cognitive side effects all occur. They’re classified together with benzodiazepines in most prescribing studies because the harm profiles overlap substantially.
Is psychotropic use without diagnosis a problem?
It depends. Symptomatic primary-care prescribing for distress is reasonable in many contexts. The concern is when it becomes long-term without periodic reassessment of whether the medication is still helping, or when it bypasses non-pharmacological alternatives that would work as well.
References
- Wessman I et al. Psychiatric health of Icelandic adults 40 years or older: a nationwide study of diagnoses, medications, and symptoms. PLoS One. 2026;21(4):e0342075. doi:10.1371/journal.pone.0342075
- Olfson M, King M, Schoenbaum M. Benzodiazepine use in the United States. JAMA Psychiatry. 2015;72(2):136-142. doi:10.1001/jamapsychiatry.2014.1763
- Pottegård A, Friis S, Andersen M, Hallas J. Use of benzodiazepines or benzodiazepine-related drugs and the risk of cancer: a population-based case-control study. Br J Clin Pharmacol. 2013;75(5):1356-1364. doi:10.1111/bcp.12001
- Markota M, Rummans TA, Bostwick JM, Lapid MI. Benzodiazepine use in older adults: dangers, management, and alternative therapies. Mayo Clin Proc. 2016;91(11):1632-1639. doi:10.1016/j.mayocp.2016.07.024
- GBD 2019 Mental Disorders Collaborators. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990–2019. Lancet Psychiatry. 2022;9(2):137-150. doi:10.1016/S2215-0366(21)00395-3